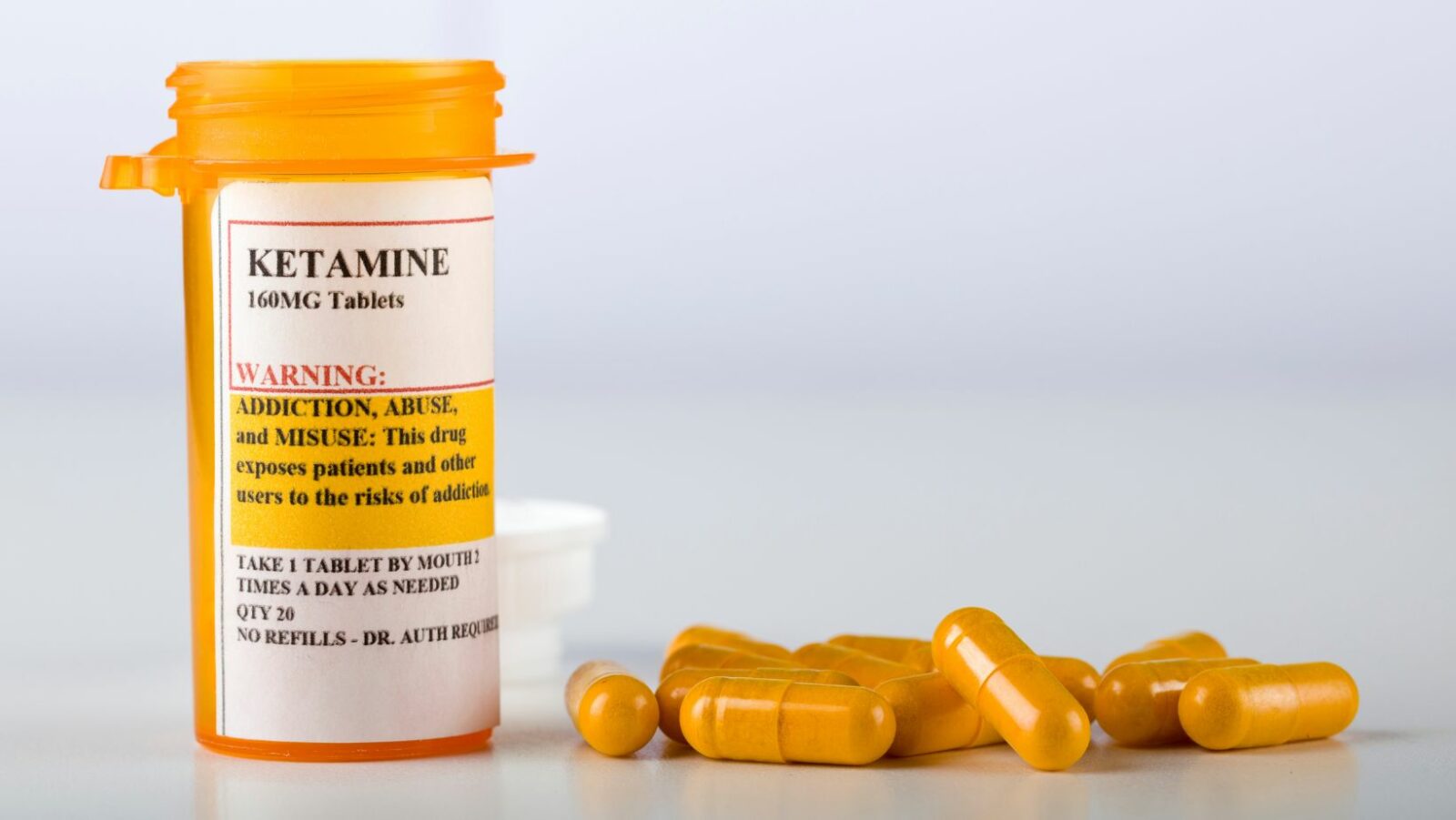
Postnatal depression (PND) is a common disease that affected many new mothers in their early baby life which can have drastic effect on their mental health and can decrease their abilities. However, recent research suggests that there may be new hope on the horizon for preventing and treating PPD using an unexpected candidate: “Space Oddity.” In the following piece of writing, we will focus on the good news on the horizon, which is ketamine as a potentially groundbreaking solution to the ever-pressing postpartum depression problem, ponder the relevance of such a remedy for maternal mental health now and in the years to come, and finally take a glance at the future of this new strategy.
Understanding Postpartum Depression: A Silent Struggle for Many Mothers
Postpartum depression is called a type of mood disorder to be mindful in it of new moms after childbirth as a rule under a few weeks or months of delivery. Symptoms of PPD differ between individuals but they usually include: sadness, anxiety, irritability, not being able to connect well with their child from attachment. PPD is just not another name for baby blues. Left untreated, it can pose a serious threat to both the mother and her newborn, and thay is apparent in how she relates to her new baby, how she breastfeeds and recovers, and how her family is faring.

In spite of the certainty of the production of and effect of postpartum depression, the treatment choices probably insufficiently, leading to consequences in which a great deal of women suffer in a lonely way. Conventional remedies like antidepressants and psychotherapy may not suit all women and it is possible for a couple of weeks to go by without any effect of these treatments being felt but this delay can result in a critical gap in care and support for mothers experiencing such conditions.
Ketamine: From Anesthesia to Antidepressant
Ketamine, which is frequently used for its great anesthetic and party drug effects, has received recent attention because it can instantaneously function as an antidepressant. The very particular way how ketamine affects the brain is not completely revealed yet, but what is certain is that it works by obstructing some receptors while helping new connections in the brain grow more rapidly. Consequently, the symptoms of major depressive disorder as well as other mental health disorders can be relieved.
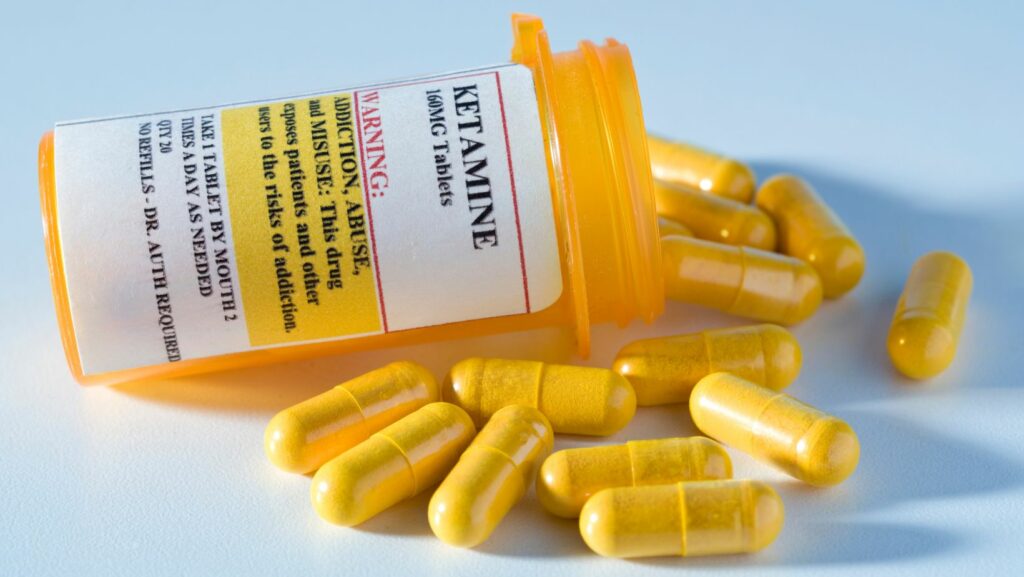
Ketamine has been looked into by researchers with us in the postpartum depression as a I case of ketamine being used as a preventative I treatment of existing I symptoms. The healthcare providers trying to do so they administer ketamine process quickly after the childbirth with the aim to purposefully shield from the development of the PPDD, the more intensive intervention requiring.
Promising Research: Early Findings on Ketamine for PPD Prevention
Preliminary trials on administering a single dose of ketamine within 2-3 days after delivery have been beneficial and effective, with the ketamine therapy exhibiting a fairly substantial decrement in the risk of developing PPD. Ketamine placebo-controlled study published in [Journal Name] found that those women who received ketamine within 24 and a half hours of their delivery of a child were less likely to display symptoms of depression in the short aftermath of the delivery as compared to those women who received placebos.
These results, therefore, offer hope for women at risk of postpartum depression, as the method described may one day result in a highly effective novel practice of curing this distressing condition. Through various mechanisms and by acting before the brain cells and other important system change during the critical initial postpartum period, ketamine could offer an alternative and practical option for mental health promotion in this difficult period.
The Future of Ketamine for Postpartum Depression Prevention
Although the precise research on using ketamine for the depression prevention in postpartum is just at the early stage and the results hardly publicized, however, those initial results stand out a good fact in front of others, indicating a good potential of the research for the future of maternal health care. As the process of disclosure is important in mitigating the impact of trauma, clinicians and researchers may explore the value of exposure to effective treatments, such as ketamine, in the prevention of postpartum depression while improving the quality of life in new motherhood.
But its vital to go slowly and do in depth research before deciding on the applicability of ketamine into prevention of postpartum depression. Comprehensive partnership among academic, clinical, and maternal health professionals would be playing a vital role in exploring the nitty-gritty of the new treatment option and enabling availability, safety and effectiveness of the treatment to reach women who need it.
Conclusion
At last, ketamine becomes the likely preventive option for postpartum depression that provides new hope to mothers who have entered the postpartum period. Although additional studies are necessary to demonstrate the strong point of these findings, optimizing treatment modalities and providing protection against the negative consequences of PPD for women may be the beginning of a significant step forward in maternal health care.